Prevent Blood Clots in Your Legs by Staying Mobile
They call it “economy class syndrome.” It occurs when blood clots form in the veins of your legs and other parts of your body as you fly for hours in the cramped seating of economy class. But, the lack of leg room isn’t necessarily the reason why you might develop blood clots in coach. More likely, keeping your legs (and the rest of your body) immobile for hours is to blame, whether you’re cramming yourself into coach, flying with style in business class, or assuming a “crash position” as a couch potato at home.
A number of factors can increase your risk of developing these dangerous blood clots, a condition known medically as deep vein thrombosis (DVT). Before you climb into coach for a long flight or relax for hours on your recliner, understand what causes DVT, as well as what you can do to prevent the life-threatening complications that can result from it.
Get Your Nutrition Guide
Do you want to eat foods that help you feel better, stay slim, and avoid diet-related diseases? Do you want to be healthier by eating delicious “super” foods?
If so, claim your FREE copy, right now, of the definitive nutrition guide on living a longer, healthier, happier life.
Bad Blood Clots
As its name implies, deep vein thrombosis is a condition in which one or more blood clots develop in a deep vein, usually in your legs. Once there, a DVT can cause symptoms such as swelling, pain, a warming sensation, and skin discoloration (redness) in the affected leg. However, some people with DVT experience no obvious symptoms.
Sitting in economy class, in and of itself, is not the reason why a DVT occurs, as 2012 guidelines from the American College of Chest Physicians (ACCP) assert. Rather, among other reasons, venous blood clots develop because you don’t move, causing your blood to stagnate and creating an environment conducive for the formation of blood clots.
“Traveling in economy class does not increase your risk for developing a blood clot, even during long-distance travel; however, remaining immobile for long periods of time will,” ACCP guideline co-author Mark Crowther, MD, of McMaster University, Ontario, Canada, said in a statement. “Long-distance travelers sitting in a window seat tend to have limited mobility, which increases their risk of DVT. This risk increases as other factors are present.”
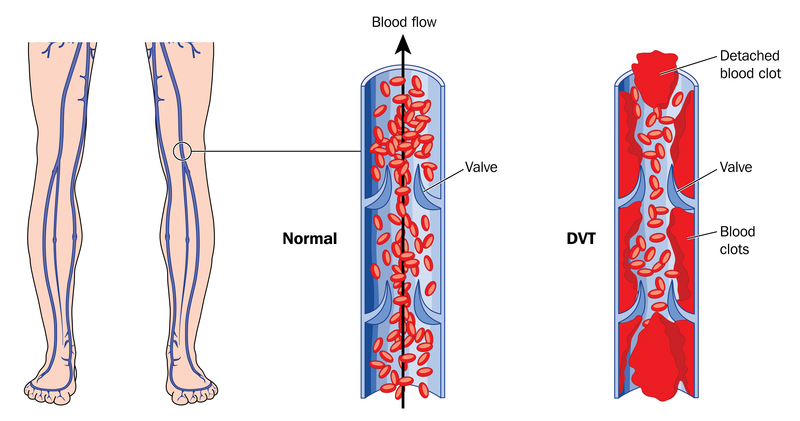
The image here illustrates the interruption in blood flow resulting from deep vein thrombosis. (Illustration: Legger | Dreamstime.com)
In addition to immobility, several factors increase the likelihood that you’ll develop a DVT during air travel:
- Advancing age (higher risk for people over age 60)
- Obesity
- A personal or family history of DVT or certain clotting disorders known as thrombophilia
- Pregnancy
- Use of estrogen (hormone replacement therapy) or birth control pills
- Certain cancers (and medications used to treat them)
- Recent surgery or trauma
- Chronic inflammatory diseases, such as inflammatory bowel disease
- Cardiovascular risk factors, such as diabetes, high blood pressure, and abnormal cholesterol levels
- Heart failure
- Smoking
The Complications of DVT
The most dangerous complication of DVT is known as pulmonary embolism, or PE. This life-threatening condition occurs if blood clots travel from the leg to the veins of the lungs. Once there, they can block blood flow and cause symptoms such as sudden shortness of breath, lightheadedness, chest pain that worsens with deep breathing or coughing, increased heart rate, and coughing up blood. A PE should be treated as a medical emergency. If you experience these symptoms, call 911 immediately.
Another, more common complication of DVT is post-thrombotic syndrome (postphlebitic syndrome), which results from damage to the vein and reduced blood flow caused by the offending blood clots.
Occurring in nearly half of DVT patients, post-thrombotic syndrome can cause chronic pain, tingling and swelling in the affected leg, a feeling of heaviness in the leg, skin discoloration (usually a brownish hue), itching, skin sores, hardening of the skin, and skin ulcerations. If it does develop, post-thrombotic syndrome usually occurs within six months of a DVT episode, although some people may develop it a year or two later.
DVT Treatment
Anticoagulant medications (blood thinners) can halt further growth of existing blood clots, keep subsequent clots from developing, and help prevent a DVT from traveling to the lungs and causing PE. These drugs may be given intravenously (heparin) or as an injection: heparin, fondaparinux (Arixtra), enoxaparin (Lovenox) and dalteparin (Fragmin). For severe clots, an intravenous “clot-busting” drug known as a tissue plasminogen activator may be administered to break up the clot.
Furthermore, you may be prescribed an oral anticoagulant, such as the widely used blood thinner warfarin (Coumadin). More and more, physicians are turning to a newer class of medications known as direct oral anticoagulants (DOACs), which include apixaban (Eliquis), dabigatran (Pradaxa), edoxaban (Savaysa), and rivaroxaban (Xarelto).
Although the DOACs offer more convenience to patients and do not require the strict monitoring of warfarin, they’re not for everyone. Each oral medication has advantages and disadvantages that you should carefully review with your physician.
Preventing Venous Blood Clots
If you’re at increased risk of DVT and PE, take steps to reduce your risk, especially while on a long flight. Ask your doctor about graduated compression stockings, which help promote better blood flow and may reduce the risk of DVT and post-thrombotic syndrome. If your risk of DVT and PE is particularly elevated, discuss with your physician whether you should take preventive anticoagulant therapy.

You know the feeling…. But before a long flight, specify to flight attendants your need to get up and move around sporadically to avoid being in a cramped position for hours.
Aboard the plane, choose an aisle seat, and get up frequently and walk around. While you’re sitting, draw circles with your feet and stretch your calf muscles.
Do those same leg exercises when you’re on long road trips, as well. And, make frequent rest stops so you can get out and stretch your legs.
If you’re undergoing surgery, talk to your doctor about medications to prevent blood clots, especially if you’ll be immobilized after your operation. Ask if a nurse or a physical therapist can help you do range-of-motion exercises with your legs to help reduce the risk of clot formation.
Most important, address important lifestyle factors that heighten your risk of developing blood clots. If you’re overweight or obese, work with your healthcare team to shed pounds with a proper diet and appropriate exercise. (See our posts “The Benefits of Walking” and “Yoga for Beginners” for motivation to stay active.) If you smoke, talk to your doctor about nicotine replacement therapy, medications, counseling, and other strategies to help you quit.
The post Prevent Blood Clots in Your Legs by Staying Mobile appeared first on University Health News.
Read Original Article: Prevent Blood Clots in Your Legs by Staying Mobile »
Powered by WPeMatico



