6. Disorders of the Gallbladder
The gallbladder is a small, pear-shaped pouch that sits next to the liver and aids in the process of digestion.
The liver produces a fluid called bile, which is a combination of water, bile acid, cholesterol, bilirubin, and lecithin. Bile helps digest fats in the small intestine. Once the bile is produced, it is stored in the gallbladder until it is needed in the small intestine. When you eat foods containing fat, the gallbladder sends bile through a system of tubes (ducts) that lead into the small intestine, where the bile salts break up (emulsify) fat.
Gallstones
If there’s too much cholesterol or bilirubin in bile, solid crystals can form in the gallbladder and clump together into gallstones. About 80 percent of gallstones are composed of cholesterol. The remaining stones—called pigment stones—are small, dark stones made of bilirubin. Gallstones can vary in size from as small as a grain of sand to as large as a golf ball.
When gallstones remain in the gallbladder, they do not cause symptoms. Some gallstones may be small enough to travel into the small intestine without causing any discomfort. Problems occur when a gallstone is large enough to block the normal flow of bile through the ducts (see Box 6-1, “Gallstones, and Locations Where Ducts Can Be Blocked,” on page 53). The hepatic ducts carry bile out of the liver, the cystic duct takes bile to and from the gallbladder, and the common bile duct takes bile from the cystic and hepatic ducts to the small intestine. If a gallstone gets caught in the cystic duct, trapping bile, the gallbladder can become inflamed. This condition is called cholecystitis.
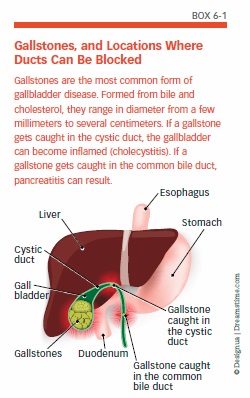
The pancreas also produces digestive enzymes that travel to the small intestine through the pancreatic duct. The pancreatic duct joins the common bile duct as they enter into the intestine. If a gallstone becomes lodged in the common bile duct, it can trap digestive enzymes in the pancreas, causing a condition called pancreatitis.
Women between the ages of 20 and 60 are two to three times more likely to develop gallstones than men. After age 60, the disparity between men and women disappears, and adults of both genders are more likely to develop gallstones than younger adults. Excess estrogen appears to increase cholesterol levels, which may explain why women taking birth-control pills or hormone therapy are at increased risk.
Other factors that raise the risk of developing gallstones include being overweight, losing a lot of weight quickly, fasting, and having diabetes. One study found that childhood obesity might increase the risk of gallstones. There are also hereditary factors: Native Americans and Mexican-Americans have a particularly strong genetic predisposition to developing gallstones, but anyone with a family history of gallstones may also be at increased risk.
Recent research suggests that women who consume large amounts of carbohydrates (found in bread, rice, potatoes, pasta) and fructose (found in fruits and sodas) are at higher risk for developing gallstones during pregnancy. A plant-based diet rich in fiber and magnesium found in whole grains, green vegetables, legumes, nuts, and seeds may reduce the risk of gallstones.
Gallstone Symptoms
Symptoms often occur suddenly after eating a fatty meal. Pain results from spasms of the gallbladder as it tries to push the bile through the duct that is obstructed by the stone. The most common symptoms include:
- Severe pain in the upper-right side of the abdomen (called biliary colic) that waxes and wanes, and lasts from 30 minutes to several hours
- Pain that radiates to the back, between the shoulder blades and under the right shoulder
- Nausea or vomiting
If the stone is stuck in the common bile duct, bile can back up and enter the blood, causing jaundice, a condition in which the skin and whites of the eyes appear yellow. If the above symptoms are accompanied by the following symptoms, a trip to the doctor or Emergency Department is needed right away:
- Sweating
- Chills
- Low-grade fever
- Jaundice
- Clay-colored stools
- Dark yellow urine
Diagnosing Gallstones
When gallstones remain in the gallbladder, they don’t interfere with the function of the gallbladder, liver, or pancreas, and don’t cause symptoms. Therefore, there’s no need to treat them. If symptoms occur, however, an ultrasound scan will be ordered to make the diagnosis. Other tests that may be done include a CT scan, MRI scan, cholescintigraphy, endoscopic ultrasound, or endoscopic retrograde cholangiopancreatography (ERCP). Blood tests may also be ordered to look for signs of infection, obstruction, or jaundice.
Treating Gallstones
If the pain from gallstones is mild and intermittent, simply avoiding fatty foods may prevent or reduce it. If the symptoms are more severe, or fever suggests acute inflammation, the gallbladder may need to be removed (see Box 6-2, “Laparoscopic Procedure Useful in Treating Gallstones”).

Gallbladder removal is one of the most commonly performed surgical procedures in the United States. It is usually accomplished with a procedure called laparoscopic cholecystectomy, which requires only small incisions, and produces minimal scarring. The surgeon makes several small incisions in the abdomen and inserts a tube tipped with a lens through one of the slits, and surgical instruments through the others. The surgeon guides the instruments while watching the image on a video monitor. The gallbladder is removed through one of the small incisions.
Sometimes an infection or scar tissue from previous operation makes it impossible to continue with laparoscopy. If this happens, the surgeon will make a five- to eight-inch incision in the abdomen to remove the gallbladder. This is required in only about 5 percent of gallbladder removals. However, obesity may increase the rate that laparoscopic cholecystectomy must be converted to open surgery.
After cholecystectomy, more than 99 percent of patients have no further symptoms. The gallbladder is not missed, because it only functions as a storage facility—without it, bile flows directly from the liver to the small intestine.
After having their gallbladder removed, people are advised to stay on a low-fat diet, eat small meals, and reintroduce high-fiber foods slowly to avoid cramping.
The post 6. Disorders of the Gallbladder appeared first on University Health News.
Read Original Article: 6. Disorders of the Gallbladder »
Powered by WPeMatico
