1. Understanding Your Brain
There is surprising good news about the brain and degenerative diseases that can affect it: Predictions that rates of Alzheimer’s disease and other dementias will explode as the nation’s population ages may have been too pessimistic. According to a study published in 2017 in JAMA Internal Medicine, rates of dementia have actually declined in recent years. Moreover, when people do develop dementia, it is striking at an older age.
Research on 21,000 Americans, ages 65 and older, representing all races, education, and income levels, looked at participants in the Health and Retirement Study. The study found that the rate of dementia fell by 24 percent over 12 years, from 11.6 percent in 2000 to 8.8 percent in 2012. Additionally, the average age of dementia diagnosis increased over the same period from 80.7 years old to 82.4.
“The dementia rate is not immutable,” says Richard Hodes, MD, director of the National Institute on Aging, which funded the study. “It can change.”
A few smaller, more homogeneous studies had shown similar encouraging signs, but an Alzheimer’s Association spokesman said experts had previously been reluctant to draw conclusions based on such limited data. Now, Keith Fargo, PhD, director of scientific programs and outreach, says of the new data, “Here is a nationally representative study. It’s wonderful news.” The findings suggest that roughly a million and a half people ages 65 and older who do not have dementia now would have had it if the rate in 2000 had continued unchanged.
Lifestyle, Not Drugs
What’s behind this good news? Experts aren’t certain, but it is not due to any breakthroughs in pharmaceutical interventions against Alzheimer’s. In fact, even as dementia rates have been declining, the news about medicines to treat the condition has been almost uniformly negative.
“’The history of the results of clinical trials has been a history of disappointment,” Dr. Fargo acknowledges. The FDA has approved only four drugs for the treatment of Alzheimer’s disease—donepezil (Aricept), galantamine (Razadyne), memantine (Namenda), and rivastigmine (Exelon) Thus far, clinical trials using these drugs have had a 99 percent failure rate, Since 2003, only one new Alzheimer’s therapy, Namzanic—a combination of two previously approved drugs, donepezil and memantine—has won federal approval.
Instead, experts on aging believe that improved understanding of the brain, coupled with a population better informed about health and nutrition, can help reduce the toll of Alzheimer’s and dementia as the nation ages. Evidence shows, for example, that people who take steps to control their blood pressure and cholesterol have a lower incidence of dementia.
Other research suggests that it’s never too early to start taking better care of your brain. A 2015 study published in the journal Brain reported that the changes in the brain associated with Alzheimer’s disease may be detectable years before the onset of the disease, even in people as young as 20. The findings imply that Alzheimer’s disease is truly a lifelong process and that preventive interventions may need to begin much earlier.
What’s Normal?
It’s true that occasional lapses in memory occur more frequently as people get older. Memory loss and other signs of cognitive decline are not inevitable, however. The serious cognitive losses associated with Alzheimer’s disease and other types of dementia are not natural parts of aging. Forgetting where you put your car keys or slipping on a person’s name is normal; putting your keys in the stove or being unable to recognize your grandchildren is not.
While some risk factors for Alzheimer’s and other forms of dementia, such as genetics, are beyond your control, the good news is that there is much you can do to preserve and even improve your “brain power.”
Your Amazing Brain
The human brain weighs only about three pounds, yet manages to carry on thousands of chemical reactions every second. Although on average the brain makes up only two percent of a person’s body weight, your hard‑working brain consumes 20 percent of the oxygen you breathe and 20 percent of the energy you take in from food.
To understand how the brain works, think of it like a baseball team (see “The Brain,” Box 1-1). Each specialized part of the brain—like the pitcher, catcher, shortstop, and others on a baseball team—performs a specific job. If any one part of the team fails, such as a pitcher serving up a “gopher” ball or a shortstop bobbling a fielding play, a whole inning can be lost.
The hindbrain, which includes the upper spinal cord, brainstem, and cerebellum, controls the body’s vital functions, such as heart rate and breathing. The cerebellum also manages movement and the actions your body has “memorized,” such as swinging a golf club or playing the piano. The midbrain, the uppermost part of the brainstem, controls some of your reflexes and is part of the process that coordinates eye movements and other voluntary motions.
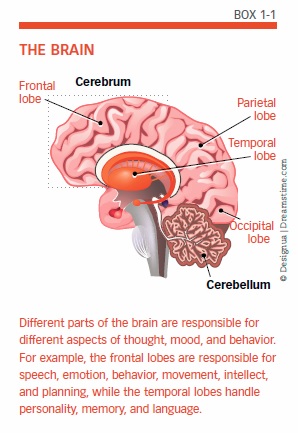
Where Thinking Happens
The cerebrum, part of the forebrain that is located at the top of the brain, is the site of those activities we broadly call “thinking.” When you read a newspaper, play bridge, write an email, or recognize a friendly face, your cerebrum is at work. It stores your memories and enables you to plan and carry out those plans—what cognitive scientists call “executive function.”
You’ve probably also heard the terms “left brain” and “right brain,” which refer to the cerebrum’s two hemispheres. Each hemisphere specializes in certain kinds of tasks the brain performs: Typically, the right side of the brain is responsible for more creative functions, while the left hemisphere performs grammar, vocabulary, and logical chores. However, both hemispheres actually contribute to many of these processes.
Each hemisphere controls the opposite side of the body, with nerve signals crisscrossing between the brain’s right hemisphere and your left hand, and vice versa. So when one side of the brain is damaged, such as by a stroke or traumatic injury, it’s the opposite side of the face and body that may droop or be paralyzed.
Lobes at Work
The lobes of the brain handle additional specific tasks. The frontal lobes, located behind the forehead, take charge of planning, weighing alternatives, and envisioning possible consequences. One way they seem to do this is by temporarily storing options and thoughts you are considering (“Hamburgers tonight … or pizza?”) in working memory.
At the back of each frontal lobe, a motor area helps manage voluntary movement. Nearby, in the left frontal lobe, Broca’s area is responsible for turning your thoughts into words.
The parietal lobes, located behind the frontal lobes, handle sensory input and are also important for math and reading. The occipital lobes, at the back of the brain, process images from the eyes. The temporal lobes, located under the parietal and frontal lobes, perform similar chores with input from the ears, as well as integrating sensory information and memories.
Deeper in the Brain
Farther inside the brain, several interior structures, including the thalamus and basal ganglia, act as mediators between the cerebral hemispheres and the spinal cord. The hypothalamus, also in the interior of the brain, is important for maintaining your sleep/wake cycle, food and water intakes, and responses to stress.
Deep inside the brain, the hippocampus is important to your brain far out of proportion to its size. Acting as a sort of a hard drive for your memories, the hippocampus “indexes” your memories and sends them to other parts of the brain when needed.
Grey and White Matter
You’ve likely also heard of the brain’s “grey matter,” which refers not to the whole brain but rather only to the coating of the surface of the cerebrum and cerebellum. This coating is about an eighth of an inch thick—sort of like the bark on a tree. Formally called the cerebral cortex—from the Latin for “bark”—it really is grey. That’s because the cortex lacks a white insulating material called myelin that is found elsewhere in the brain; this myelin sheath allows electrical impulses to transmit quickly and efficiently along nerve cells.
Myelin makes most of the brain white, so you will also see references to “white matter.” The cortex also is famously wrinkled, and these folds serve a purpose: Much of the brain’s information processing occurs in the cerebral cortex, and its wrinkles create more surface area for this processing.
Neurotransmitters
All the various parts of your brain, large and small, communicate with one another and with the nervous system throughout your body using tiny electrical impulses along with chemical signals called neurotransmitters. Zooming in to the microscopic level, thinking and other functions of the brain and nervous system are performed by cells called neurons (see “Message Passing Across a Synapse,” Box 1-2). An adult brain contains approximately 100 billion neurons, with branches that connect at more than 100 trillion junction points called synapses.

Neurons consist of several parts: the cell body, which includes the nucleus and most of the molecules that keep the neuron alive; dendrites, which act like telegraph wires bringing data from other neurons; and axons, which carry the signals away to other cells in the body.
When a neuron is activated, a small difference in electrical charge—called an action potential—is created by the concentration of electrically charged atoms (ions) on the cell membrane of an axon. This charge zooms rapidly down the axon until it comes to the end junction point, the synapse. In most neurons, the action potential then causes the release of a neurotransmitter. This chemical message travels across the minute gap of the synapse. On the other side of the synapse, the neurotransmitter binds to receptors on the dendrites of the receiving neuron. The signal then continues in the same way from one neuron to the next, via electrical charges and neurotransmitters.
Ultimately, when the message reaches its destination, a neurotransmitter might set off a fresh chain of messages along the neurons. Or the result could be the stimulation of another kind of cell, such as those found in glands. When your body sends a “fight or flight” signal, for example, neurotransmitters wind up triggering the adrenal gland.
When Neurotransmitters Go Awry
Most of the time in healthy people, the messaging of neurotransmitters proceeds without any glitches and without our even being aware of what’s happening. When things go wrong, however, malfunctions of these neurotransmitters are associated with certain diseases of the brain. For example, a characteristic feature of Alzheimer’s disease is a reduction in levels of acetylcholine, a neurotransmitter involved in memory.
Parkinson’s disease is linked to low levels of dopamine, a neurotransmitter important in controlling movement. When the body lacks adequate amounts of dopamine, the result can be tremors, shaking, stiffness, and other symptoms characteristic of Parkinson’s disease.
Dopamine also affects the reward systems in the brain and assists in the flow of information to the front of the brain, where thinking and emotions reside. So research has also suggested that low levels of dopamine or issues with utilizing dopamine in these parts of the brain might be factors in attention-deficit/hyperactivity disorder (ADHD).
Mental illnesses can also be associated with neurotransmitter problems. For example, another neurotransmitter, serotonin, works to help control functions, such as sleep, mood, and appetite. People who suffer from depression often suffer from lower than normal levels of serotonin. That’s why the most commonly prescribed medications to treat depression are called selective serotonin-reuptake inhibitors (SSRIs): They work by blocking the automatic “reuptake” of serotonin, in which the sending neuron recycles the serotonin used to cross a synapse. That leaves more serotonin to bind onto the receiving neuron, encouraging more normal functioning and moods.
Some studies have pointed to a role for inadequate or ineffective amounts of dopamine in the development of another mental illness, schizophrenia.
Neurotransmitters and Alzheimer’s
Where other brain conditions may be caused in part by problems with neurotransmitters, Alzheimer’s disease also disrupts the normal functioning of these chemical messengers and the cells they affect. The disease damages the brain’s communications system by actually destroying synapses and killing neurons.
Some of the FDA-approved medications for the treatment (but not cure) of Alzheimer’s disease work by trying to counter these communication breakdowns. According to the Alzheimer’s Association, current FDA‑approved Alzheimer’s drugs support this communication process through two different mechanisms:
- Cholinesterase inhibitors (donepezil, galantamine, rivastigmine) work by slowing down the process that breaks down acetylcholine.
- Memantine is an NMDA (N-methyl-D-aspartate) receptor antagonist, which works by regulating the activity of glutamate. By partially blocking NMDA receptors, the drug prevents the excess release of glutamate from damaged cells. Too much glutamate lets excess calcium enter cells, which can trigger further damage.
Brain Misconceptions
Contrary to the common misperception that neurons can only form new connections during early brain development, the brain actually continues to change in response to new inputs—a characteristic called plasticity. Even adult brains can form new neuronal connections, strengthen existing ones, or eliminate old ones as you continue to gather new knowledge and experiences. Stimulating neurons can cause them to grow and form new synaptic connections, while those that go without stimulation may weaken.
This plasticity helps explain why practicing a task, such as learning to play a musical instrument, helps a person perform that task better and more efficiently. Doing something over and over again strengthens the synapses involved in that task—like paving a road to make repeated journeys go more smoothly.
Symptoms of Dementia and Alzheimer’s
Symptoms of Alzheimer’s disease and other forms of dementia occur when things go wrong in the brain. These symptoms of a decline in cognition—what we loosely call thinking and memory—affect a person’s ability to conduct everyday activities. The umbrella term for a wide range of such symptoms is “dementia,” which is not a specific disease or single condition. The best-known form of dementia, Alzheimer’s disease, accounts for 60 to 80 percent of all cases.
The earliest signs of dementia may be what’s called mild cognitive impairment (MCI), a stage between normal forgetfulness due to aging and more serious cognitive decline (see “Symptoms of Mild Cognitive Impairment,” Box 1-3). Mild cognitive impairment manifests as problems with thinking and memory that do not interfere with everyday activities. People with this condition are often aware that they are showing signs of impairment. Not everyone who develops mild cognitive impairment progresses to Alzheimer’s or other dementia.

Symptoms of Dementia
Many of the first symptoms of actual dementia, such as being unable to come up with a word that’s on the tip of your tongue or misplacing things, are common in everyday life for people who are perfectly normal. (see “Early Signs of Dementia,” Box 1-4). Many of these early signs of actual dementia are also similar to the symptoms of mild cognitive impairment. To be considered dementia, at least two of these core mental functions must be significantly impaired:
- Ability to focus, pay attention
- Communication, language
- Memory
- Reasoning and judgment
- Visual perception
As dementia worsens, symptoms grow more obvious and interfere with the ability to take care of oneself and conduct everyday life. People with severe dementia may no longer be able to perform basic activities of daily living, recognize family members, or even understand language.
Diagnosing Alzheimer’s
The earliest stages of Alzheimer’s may begin as many as 20 years before the disease is severe enough to be diagnosed. When Alzheimer’s strikes relatively younger people, it may not be characterized by the memory problems we associate with the disease. A study published in the November 2015 issue of Alzheimer’s & Dementia stated that tests for non‑memory cognitive problems should not be overlooked when screening for Alzheimer’s.
In mild and moderate stages of Alzheimer’s, the growing plaques and tangles impair mental functions enough to affect everyday activities and to be noticed by loved ones. This is when the disease is most often diagnosed (see “10 Warning Signs of Alzheimer’s,” Box 1-5).
Alzheimer’s Brain Changes
Unlike dementia in general, Alzheimer’s disease is associated with specific changes in the physical condition of the brain. A brain affected by Alzheimer’s has far fewer nerve cells and synapses than a healthy brain. The “grey matter” actually begins to shrivel, impairing the ability to process information. The hippocampus, so important to the formation of new memories, shrinks. Fluid-filled spaces within the brain, called ventricles, grow larger.
When reading about Alzheimer’s disease, you’ll see references to two types of characteristic brain formations, called plaque and tangles. Plaque is formed when pieces of a “sticky” protein called beta-amyloid, which comes from fatty membranes that surround nerve cells, clump together. Scientists suspect that larger plaques may not be as damaging to brain function as smaller clumps of beta-amyloid that block the messaging between the brain’s synapses.
Tangles are like traffic jams in your brain. In a healthy brain, parallel strands of “tau” proteins function like highways, carrying essential nutrients. In Alzheimer’s patients, tangles of collapsed tau block the orderly flow along the highways that serve the brain. Eventually, the cells deprived of nutrients die.
As these plaques and tangles spread through the grey matter of the brain, Alzheimer’s disease progresses. Typically, plaques and tangles strike first in areas important to learning, memory, thinking, and planning.
Picturing the Brain
At one time, the diagnosis of Alzheimer’s disease could be definitively confirmed only after death, via autopsy. But today, new imaging techniques make it possible to see the damage the disease causes in a living brain and to better understand how healthy brains function.
More detailed pictures of the brain, without the use of X-rays, can be obtained by magnetic resonance imaging (MRI). This technology takes advantage of the fact that hydrogen atoms in the brain can be affected by rotating a powerful magnet around a person’s head; the resulting changes in these atoms’ energy levels can be captured to create detailed images. Both CT (computed tomography) and MRI scans are static—like snapshots of the brain.
Links Between Heart and Brain
The brain is fed by one of the richest networks of blood vessels in the body, so changes in your cardiovascular system affect brain function—with important consequences for protecting your aging brain. Every heartbeat carries roughly one-fifth to one-quarter of your blood supply to the brain, and an even greater percentage when your brain is working hard.
Recent research has suggested that a healthy heart and blood pressure in midlife might be associated with brain volume decades later. An observational study of 1,094 participants in the Framingham Offspring cohort compared results from a treadmill test when the volunteers were about age 40 with brain volume almost 20 years later, measured by MRI scans. Participants with initial lower cardiovascular fitness and elevated blood pressure and heart rate responses subsequently averaged smaller brain volumes. Researchers said the findings linked “fitness over the life course to brain health in later life,” adding, “Promotion of midlife cardiovascular fitness may be an important step toward ensuring healthy brain aging in the population, especially in pre-hypertensive or hypertensive individuals.” Of course, since this was an observational study, it could also be that the association goes the other way, and a healthy brain contributes to cardiovascular health.
Blood Vessels and the Brain
Vascular dementia, the second-most common form of dementia after Alzheimer’s disease, begins with blood vessel damage in the brain: A stroke or a series of tiny strokes cuts off or restricts the flow of blood to brain cells, interfering with their ability to communicate with other brain cells. That in turn affects everything from your ability to think to your emotions. Vascular dementia may manifest in different ways, depending on which areas of the brain suffer damage.
Blood-vessel changes can also increase the degree of impairment or the speed of cognitive decline in other forms of dementia, such as Alzheimer’s, or a condition known as Lewy-body dementia.
Heart-Brain Health
These connections mean that many of the ways in which you can protect your brain also benefit your heart, and vice versa, because a healthy brain depends on a healthy cardiovascular system. Although you can’t control some risk factors for Alzheimer’s and other dementias, others you can. In particular, you can help protect your brain by improving your cardiovascular health with these steps:
- Keep your blood-cholesterol levels healthy by cutting down on saturated and trans fats and, if prescribed by your doctor, taking cholesterol-lowering drugs, such as statins.
- Replace unhealthy fats with unsaturated fats; current evidence suggests that polyunsaturated fats, found in liquid vegetable oils and nuts, are the most heart-healthy choice, though other benefits have been associated with monounsaturated fats, found in olive and canola oils and avocados.
- Control your blood pressure by reducing salt intake, following a healthy diet (the DASH eating plan is specially formulated to combat hypertension), and taking blood-pressure medications if prescribed by your doctor.
- If you smoke, here’s another reason to quit; if you don’t smoke, don’t start.
- Follow a heart-healthy diet, such as DASH (see above) or a Mediterranean-style diet, which we’ll explore in the next chapter.
- Maintain a healthy weight.
- Maintain healthy blood-glucose levels by watching your weight and reducing intake of refined carbohydrates, starches, and sugar to avoid diabetes, which in turn contributes to heart disease.
- Follow exercise guidelines, which generally advise getting 30 minutes a day of at least moderate physical activity on most days of the week. Exercise seems to directly benefit brain health by increasing blood and oxygen flow to brain cells, and benefits your overall cardiovascular system.
As we’ll see in the rest of this Special Health Report, smart choices about nutrition and lifestyle can make a big difference. While some things about your aging brain are beyond your control, these simple steps can improve your odds.
The post 1. Understanding Your Brain appeared first on University Health News.
Read Original Article: 1. Understanding Your Brain »
Powered by WPeMatico

