1. Eating Wisely As You Age
How Diet Makes a Difference
We all know that eating a healthy diet is important for growing children, and the obesity epidemic and soaring rates of diabetes, cardiovascular disease, and other chronic diseases dramatically demonstrate the need to eat right from young adulthood into middle age. But does what you eat really matter as you grow older? Isn’t there a point in life where you can eat whatever you want?
If that’s what you think, you might want to consider a saying often attributed to pitcher Satchel Paige: “If I knew I was going to live this long, I would have taken better care of myself.” The evidence is overwhelming that the dietary choices you make as you age can improve your quality of life, as well as extend its length.
In 2013, the Centers for Disease Control and Prevention published the 10 leading causes of death for different age groups. Five of the leading causes of death for individuals over age 60 are conditions that benefit from diet and nutrition intervention: cardiovascular disease, cerebrovascular disease, type 2 diabetes, cancer, and kidney disease. Besides shortening your life, all of these conditions also affect how much you can enjoy your life.
Cardiovascular Disease
This condition that affects the heart and blood vessels is the leading cause of death in the US and around the world. Three risk factors for cardiovascular disease that are influenced by diet are unhealthy blood lipid levels (including high LDL cholesterol and triglycerides), high blood pressure (hypertension), and, of course, obesity.
Helen M. Rasmussen, PhD, RD, senior research dietitian at Tufts’ USDA Human Nutrition Research Center on Aging (HNRCA) and co-creator of MyPlate for Older Adults (a dietary plan discussed later in this chapter), points out: “Weight reduction and subsequent maintenance of normal weight for those who are overweight or obese can increase one’s enjoyment of everyday activities. Imagine carrying around a 20-pound sack of flour with you wherever you go. Once you have eliminated the baggage of extra pounds, you may feel lighter, breathe easier, and be able to get around more comfortably with less joint pain. It may even encourage you to increase your activity routine, hence improving your mobility and revving up your metabolism.”
As a bonus, she says, weight reduction can also help you get a good night’s rest, since being overweight is associated with a higher incidence of sleep apnea.
Diet and Your Brain
Cerebrovascular diseases are conditions that develop as a result of problems with the blood vessels that supply the brain. The most common types of cerebrovascular diseases are the different types of stroke. Problems with blood circulation that result in inadequate blood flow to the brain can also cause vascular dementia. The most important risk factor for cerebrovascular diseases is high blood pressure. Says Dr. Rasmussen, “Lowering dietary sodium levels has been shown to decrease blood pressure. People over the age of 50 should aim to keep their sodium intake at 1,500 milligrams per day. Although the optimal level of sodium intake is currently under debate, it is a fact that most Americans consume too much sodium, and cutting back on sodium is definitely a healthy choice.”
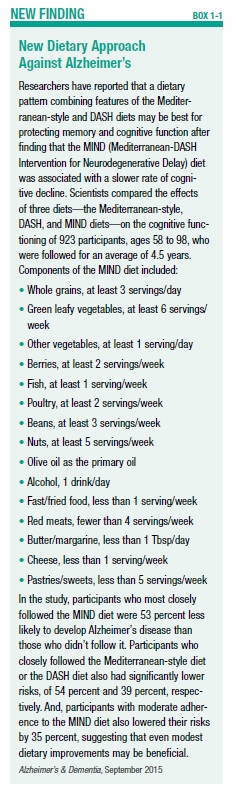
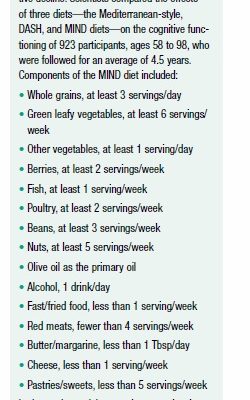
A healthy diet has also been shown to reduce your risk of Alzheimer’s disease and other forms of dementia. Both the Mediterranean-style diet and the DASH eating plan, which are discussed later in this chapter, have been associated with cognitive benefits. A hybrid of these plans that emphasizes brain-protective foods, the “MIND” diet, may be even more effective (see Box 1-1, “New Dietary Approach Against Alzheimer’s”).
Diabetes Risk
Type 2 diabetes, a condition identified by high blood glucose (sugar) levels in the bloodstream, is associated with a two to four times higher risk of death from heart disease or stroke. Other complications from diabetes include vision loss, kidney disease, and neuropathy (nerve damage, usually in the legs and feet). Maintaining a normal weight and choosing foods that do not rapidly raise blood glucose can help you control your blood glucose levels. Eating less saturated fat, avoiding high-sugar food items, and eating more fruits, vegetables, and whole grains are also recommended to help control the complications of diabetes, as well as preventing or delaying its onset.
Food and Cancer
The relationship between diet and cancer risk is less well understood, but experts advise maintaining a healthy weight, limiting red meats, and processed meats, and eating more fruits and vegetables and whole grains to reduce your risk. According to the American Cancer Society, it has been estimated that as many as one-third of all cancer deaths in the US are related to diet and activity factors.
Chronic Kidney Disease
This condition, abbreviated CKD, means your kidneys cannot properly filter waste from your blood; these waste products remain in your body and can cause health problems. The chances of developing CKD increase with age; it most commonly affects individuals age 70 and over. Those who have diabetes, hypertension, cardiovascular disease, and are obese are at risk for CKD, so a healthy diet and keeping yourself well-hydrated can reduce your risk.
Your Changing Nutrient Needs
People’s nutritional needs change with age. As activity levels decrease and muscle mass declines, older people need to consume fewer calories; some may also simply have a reduced appetite, and illness or medications can affect the appeal of food. If you’re consuming fewer calories, however, it’s more important to get the most nutritional “bang” for your caloric “buck.”
The Importance of Nutrient Density
Choosing foods high in key vitamins, minerals, fiber, protein, and other essentials means emphasizing nutrient density, rather than energy density. What’s the difference? A medium apple and an eight-ounce glass of non-diet cola both contain about 100 calories, but the apple contains fiber, vitamin C, potassium, and other nutrients—it’s more nutrient dense. The cola is energy dense—high in calories—because of its high sugar content, but it provides no healthy nutrients.
Nutrient-dense foods include fruits and vegetables, whole grains, seafood, lean poultry and meats, dairy products, and eggs. Most popular snacks such as potato chips or corn chips, sugary beverages, and baked goods made from refined grains are less nutrient-dense. In general, nutrient-dense choices are more likely to be whole foods rather than processed or refined, contain little or no added sugar or fat, and have less saturated fat for the amount of nutrients than similar products.
If you’re eating less as you get older—whether because your appetite declines or you’re avoiding obesity—make sure you’re choosing nutrient-dense foods. Eat a banana instead of a candy bar, broccoli rather than French fries, yogurt rather than a bag of chips, and whole-wheat bread instead of a white dinner roll.
Are You Getting Enough?
Another reason to make smart food choices as you get older is that you might not be getting enough of certain key nutrients. This can occur either because your body and lifestyle have changed or because your needs have increased with age. Examples include:
- Vitamin B12. The amount of B12 your body needs for proper blood-cell formation, neurological function, DNA synthesis, and other tasks doesn’t change with age, but your ability to obtain this vitamin from food might. Although B12 is a water-soluble vitamin, B12 that is naturally present in foods such as meat, fish, poultry, eggs, and dairy products is bound to proteins in the food. In your stomach, hydrochloric acid and pepsin (an enzyme that breaks down proteins) release the B12 for your body to use. But people with low levels of stomach acid, whether due to aging or the use of certain medications, can’t extract as much dietary B12. And, a condition called atrophic gastritis, which decreases the secretion of hydrochloric acid in the stomach, affects between 10 percent and 30 percent of older adults.
The vitamin B12 found in fortified foods, such as breakfast cereals, is different. The crystalline synthetic form of B12 added to foods or used in supplements is already in a free form that doesn’t require stomach acid for your body to use it. The Institute of Medicine recommends that people over age 50 obtain most of their vitamin B12 from fortified foods and supplements.
- Vitamin D. Essential for bone health and a wide range of metabolic processes, vitamin D can be difficult to obtain in adequate amounts from food alone. With age, your body also loses some of its natural ability to make vitamin D in your skin from sun exposure, and older people often spend less time out in the sun.
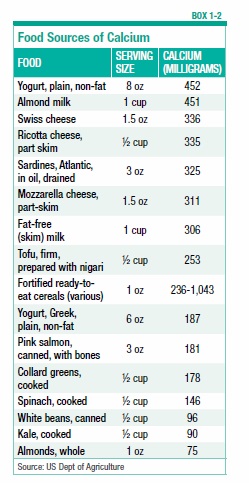
- Calcium. The amount of calcium needed to maintain bone density and prevent fractures increases for women over age 50 and for all adults over age 70. Because there are some possible side effects from high levels of calcium in supplement form, experts advise getting as much of your daily calcium needs as possible from dietary sources (see Box 1-2, “Food Sources of Calcium”).
- Iron. Once women hit menopause, their iron needs decrease to the same amount as men, but, for both genders, low stomach acid canaffect the ability to absorb iron from foods.
- Fiber. When you get older, none of the organs and organ systems in your bodies function as efficiently as they used to, including the GI tract. This means constipation is more likely; getting enough dietary fiber can help. Adequate fiber intake has also been linked to lower risks of several diseases associated with aging, including cardiovascular disease, diabetes, and colorectal cancer.
- Water. Thirst, rather than some “rule” about drinking eight glasses of water a day, is your best guide to staying hydrated. However, your sense of thirst diminishes with age, so you may need to pay closer attention to getting enough water and other healthy fluids to prevent dehydration. Water is also important when consuming fiber because it helps fiber bulk up and keep wastes moving through your intestines.
Medications and Nutrients
The medications that so many of us take as we get older can also contribute to nutrient shortfalls. In 2007 through 2010, almost 50 percent of all Americans reported taking one or more prescription drugs in the past 30 days; use increased with age, with the number climbing to 90 percent among those age 65 and over. Medications can interfere with your body’s ability to utilize nutrients by impairing digestion and the availability or storage of nutrients, as well as by increasing losses of nutrients by excretion. Among the most common medications that affect nutrition are:
- Antacids/Proton-pump inhibitors (PPIs): Taken for heartburn and indigestion, these drugs can negatively affect the absorption of vitamin B12, folic acid, vitamin C, calcium, magnesium, iron, and zinc.
- Metformin: This common diabetes medication has been shown to contribute to depletion of vitamin B12 and possibly folic acid.
- Anti-hypertensives: Medications for high blood pressure can decrease the availability and increase the elimination of zinc. They also increase the excretion of B vitamins, vitamin C, potassium, magnesium, and calcium.
- Statins: These widely prescribed cholesterol medications can increase the depletion of coenzyme Q10 and have been associated with vitamin D insufficiency.
- Bronchodilators: Used for asthma and other breathing difficulties, these increase the excretion of vitamin B6 and calcium and block vitamin D absorption.
Other Reasons for Shortfalls
There may be other reasons you’re not getting enough of the right nutrients as you age. These can include health conditions such as heartburn or reflux, poor dentition, difficulty swallowing, or nausea or loss of appetite from chemotherapy or other medical treatments. Or, you might simply be less able to or less interested in cooking or going to the grocery store, as often occurs due to factors such as reduced mobility, lack of transportation, depression, or adjusting to the loss of a spouse.
You might not even be aware that such factors are causing you to miss out on healthy eating. Friends and relatives, especially those who live far away and see you only at intervals, may be the first to notice such warning signs as weight loss or lagging appetite. Make sure to discuss any such issues with your physician, too, and use your regular physical as a check-up on your weight.
A diet with softer, less spicy, and more easily digestible foods can often address this sort of nutrition shortfall. You may want to consult a registered dietitian (RD) for help in adjusting your diet.
Do You Need Supplements?
Nutrition experts agree that the best way to get the nutrients you need at any age is by consuming a healthy diet. When individual vitamins and minerals have been tested in supplement form, the results have mostly been disappointing; this suggests that it’s difficult to replicate the benefits of the nutrient mix of whole foods. Exceptions where the evidence is clear for a benefit from supplements include the AREDS antioxidant formula for lowering the risk of macular degeneration and the fortification of foods with folic acid to reduce birth defects. As noted above, older people may also benefit from supplemental vitamin B12 or foods fortified with the supplemental form. Because it can be difficult to obtain adequate vitamin D from foods, especially in northern latitudes or with limited sun exposure, experts often suggest supplements.
What about multivitamins, which are used by about 40 percent of US adults? Multivitamin and mineral supplements can fill in the gaps and enhance the intake of problem nutrients for many Americans. Studies have shown that users of such supplements have higher blood levels of vitamins A, C, D, and E and several B vitamins, as well as lower levels of homocysteine, an important marker of cardiovascular disease. The evidence on whether taking a multivitamin actually decreases your risk of heart disease or cancer is mixed.
When choosing any type of supplement, exercise caution: Testing has revealed that some supplements contain more or less of the active ingredient(s) listed on the label and/or potentially harmful substances. Look for the “USP Verified Mark” on the label—this means the supplement has been tested by the US Pharmacopeia (see Box 1-3, “USP Verified Mark”). A USP seal ensures that the product is made in accordance with Good Manufacturing Practices, contains the ingredients listed on the package, and does not contain harmful levels of contaminants.
Supplements and “Shakes” Cautions
If you do choose to take supplements, check with your doctor first, and make sure he or she knows what you are taking. Supplements can interact with many medications. Too much supplemental calcium, particularly taken all at once rather than spread throughout the day, may increase the risk of kidney stones. If you have been diagnosed with precancerous colon polyps, limit folic acid to 400 micrograms daily, as more may contribute to cancer formation. (Since you’re also getting folic acid in fortified foods, you may want to take a multivitamin only every other day.) Beta-carotene and vitamin E beyond the amount in typical multivitamins should also be avoided.
How about drinking your nutrition in the form of a shake? The American Geriatrics Society recently advised against using the popular liquid supplements even for most older adults suffering unintentional weight loss. “There is no evidence that they affect other important clinical outcomes, such as quality of life, mood, functional status, or survival,” according to the society’s latest Choosing Wisely guidance for physicians and patients. At the society’s annual scientific meeting, Paul Mulhausen, MD, who led the Choosing Wisely work group, pointed out that such beverages’ primary ingredients are water and several forms of sugar, calling the products “liquid candy bars with vitamins.”
Make MyPlate Your Plate
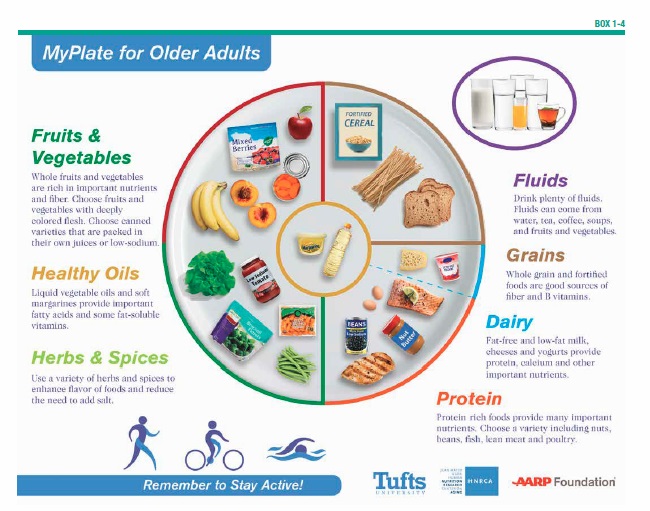
When the federal government retired its longstanding food pyramid, replacing the familiar icon with a new dietary-guidance symbol, MyPlate, Tufts nutrition scientists created a corresponding MyPlate for Older Adults. The new graphic, updated in 2016, calls attention to the unique nutritional and physical activity needs associated with advancing years. Alice H. Lichtenstein, DSc, director of Tufts’ HNRCA Cardiovascular Nutrition Laboratory, collaborated with HNRCA senior research dietitian Helen M. Rasmussen, PhD, RD, to develop it (see Box 1-4, “MyPlate for Older Adults,” on page 15).
MyPlate for Older Adults spotlights different forms of vegetables, fruits, and other healthy food choices that are convenient, affordable, and readily available. Unique components include icons for regular physical activity and emphasis on adequate fluid intake, both of particular concern for older adults. The graphic illustrates:
- Brightly-colored vegetables such as carrots and broccoli
- Deeply-colored fruits such as berries and peaches
- Whole, enriched, and fortified grains and cereals such as brown rice and 100% whole wheat bread
- Low- and non-fat dairy products such as yogurt and milk
- Protein sources such as beans and peas, nuts, fish, poultry, lean meat, and eggs
- Liquid vegetable oils, soft spreads low in saturated and trans fat, and herbs and spices to replace salt
- Fluids such as water, tea, coffee, and fat-free milk.
Each of these food and beverage groupings will be explored in depth, with spotlights on smart choices within each group and ways to include more in your diet, in subsequent chapters of this book, beginning with chapter 3.
Foods to Focus On
“Half of the MyPlate for Older Adults graphic includes fruit and vegetable icons, which reflects the importance of eating several servings of fruits and vegetables per day in a range of colors,” says Dr. Rasmussen. “Consuming a variety of produce with deeply-colored flesh, such as peaches, berries, tomatoes, kale, and sweet potatoes, introduces a larger amount of plant-based nutrients and fiber into your diet.”
Dr. Lichtenstein adds, “We also include icons representing frozen, pre-peeled fresh, dried, low-sodium, and low-sugar canned options because fruits and vegetables in these forms contain as many or more nutrients as fresh—and they are easier to prepare, are more affordable, and have a longer shelf life.”
Such factors are important to consider, she notes, when arthritis kicks in or dark, cold days mean it is less likely someone will go out to replenish the refrigerator.
MyPlate for Older Adults provides examples of whole, enriched, and fortified grains because they are high in fiber. Suggested protein sources include plant-based options, such as beans and tofu, as well as fish, poultry, and lean meat. Drs. Lichtenstein and Rasmussen recommend vegetable oils and soft spreads rich in unsaturated fats as alternatives to foods high in animal fats such as butter that are higher in saturated and trans fat.
Special Cases
Some elements of the MyPlate for Older Adults graphic factor in the special needs of older adults. “Blood pressure tends to increase as we age, so it is especially important for older adults to monitor dietary salt and, for most of us, try to find ways to decrease intake,” says Dr. Lichtenstein. “MyPlate for Older Adults suggests alternatives to salt, such as flavoring with spices, and choosing the low-sodium options of items such as canned vegetables.”
The inclusion of several examples of liquids such as water, tea, coffee, and soup addresses the common, age-related decline in thirst that can put older adults at risk for dehydration.
Also intentionally represented on the MyPlate for Older Adults are a fork and knife that serve as reminders to put down remote controls and smart phones and occupy both hands with eating utensils. Dr. Lichtenstein says, “The focus should be on the enjoyment of foods and beverages, on the amount consumed, and, whenever possible, on the opportunity for social interaction at mealtimes.”
MyPlate for Older Adults also promotes regular physical activity with icons depicting common activities that include daily errands and household chores. Although some of those chores do not take the place of more formalized exercise routines involving cardiovascular activities, those included serve to remind older adults of the variety of options for regular physical activity.
Eating Like a Mediterranean
This book largely follows the advice of MyPlate for Older Adults because this plan uniquely addresses the nutritional needs associated with aging. However, you may have also heard of other eating plans for which research has shown health benefits. For example, the so-called “Mediterranean” diet, which has been linked to reduced risks of heart disease and cognitive decline, often in appears in headlines about health and diet. We say “so-called” because there is no “official” Mediterranean diet; in fact, the Mediterranean-style dietary plans tested in research vary widely. Moreover, even in the countries bordering the Mediterranean Sea, traditional healthy ways of eating are increasingly giving way to more American-style fare, driven by convenience and economics.
A healthy Mediterranean-style diet includes many of the same key ingredients found in MyPlate for Older Adults. The chief difference between a Mediterranean-style diet and other healthy-eating plans (such as DASH, described next in this chapter) is the emphasis on unsaturated fats found in plant foods, especially monounsaturated fat in the form of olive oil. All healthy diets recommend limiting foods high in saturated fat, such as fatty meats and full-fat dairy, minimizing added sugar, and avoiding processed foods.
What “Mediterranean” Really Means
To follow a healthy diet based on Mediterranean foods, you need to know that many modern-day foods we associate with Mediterranean countries—pizza or spaghetti from Italy, moussaka or spanikopita from Greece—don’t fit in the healthy dietary plans promoted as “Mediterranean.” Take pasta as an example: Although you may think it is “Mediterranean food,” the refined grains used in familiar pasta dishes have had most of their original nutrients stripped away. Instead, healthy Mediterranean eating plans emphasize whole grains, much like the Dietary Guidelines for Americans.
The heaping helpings of cheese we associate with pasta dishes and pizza are out, too. Cheese is high in saturated fat, one of the primary elements that is minimized in a healthy diet. The unofficial but widely adopted “Mediterranean diet pyramid” promoted by the non-profit Oldways group (see Box 1-5, “Mediterranean Diet Pyramid,” on page 18) puts cheese at the top portion of the pyramid, indicating that it should be eaten infrequently and in moderate portions.
Think instead of Mediterranean fare consumed by the poorer peoples of the region. As Oldways explains, “The ‘poor’ diet of the people of the southern Mediterranean, consisting mainly of fruits and vegetables, beans and nuts, healthy grains, fish, olive oil, small amounts of dairy, and red wine, proved to be much more likely [than a ‘modernized’ diet] to lead to lifelong good health.”
For some suggestions on following a healthy Mediterranean-style diet, see Box 1-6, “Mediterranean Diet: 8 Steps to Get Started,” on page 19.
DASH to Good Health
Another healthy regimen, the Dietary Approaches to Stop Hypertension (DASH) plan, was designed by the National Heart, Lung and Blood Institute based on clinical studies that tested the effects of sodium and other nutrients on blood pressure. The first DASH study compared three eating plans: a typical American diet, the typical American diet with added fruits and vegetables, and the DASH plan. All three plans were moderate in sodium. People who followed the high fruits and vegetables plan had reduced blood pressure, and those who followed the DASH eating plan saw their blood pressure drop even more.
A second DASH study examined the effects of restricting sodium on blood pressure. The greatest blood pressure reduction occurred with the DASH plan that was lowest in sodium—just 1,500 milligrams daily.
Starting a DASH Plan
To get a healthy start on DASH-style eating, follow these simple steps:
MORE
- Fruits
- Vegetables
- Whole grains
- Nuts and legumes
- Low-fat dairy (2-3 daily servings)
LESS
- Red and processed meats
- Sweetened beverages
- Sodium
You can download the complete DASH plan for free at
http://1.usa.gov/1qvoimN.
Even if you don’t have high blood pressure, you can benefit from this healthy way to eat. In a review of six studies that examined the DASH-style diet in relation to heart health, researchers linked this dietary pattern to a 20 percent reduction in cardiovascular disease, a 21 percent reduction of coronary heart disease, a 19 percent reduction in stroke, and a 29 percent reduction in heart failure.
These findings are also powerful evidence of the ability of dietary changes to improve your quality of life and reduce your risk of life-threatening diseases. In the next chapter, we’ll show you how easy it can be to start eating better—and boosting your health—right away.
The post 1. Eating Wisely As You Age appeared first on University Health News.
Read Original Article: 1. Eating Wisely As You Age »
Powered by WPeMatico